Kartiki Churi, M.D., Family Care Center Regional Lead for Transcranial Magnetic Stimulation
Major Depressive Disorder (MDD) is a debilitating illness that significantly impacts daily activities, quality of life, cognitive function, employment status, and work productivity. As of 2020, approximately 8.4% of adults in the U.S. had at least one major depressive episode, representing an estimated 21 million Americans. At its worst, MDD can be life-threatening due to the high suicide rates.
Treatment-resistant depression (TRD) is a subset of MDD that does not respond to traditional and first-line therapeutic options. Although there is no formal consensus on the definition of TRD, it is commonly considered an inadequate response to at least two trials of antidepressant pharmacotherapy.
9 Factors that Increase the Risk of Treatment-Resistant Depression (TRD)
There is no single reason for TRD, but several factors could increase the risk of TRD, either individually or in combination.
- Co-occurring medical or psychiatric illness
- Side effects or incorrect medications
- Difficulty with treatment compliance / skipping medications
- Incorrect diagnosis
- Failing to engage in therapy
- Alcohol, cannabis, or other substance use, drug interactions
- Lack of Access to mental health services
- Genetic / Familial components
- Multiple psychiatric inpatient admissions
Risks of Untreated Depression
Research shows that depression that does not respond to typical treatment interventions carries an even higher burden of decreased quality of life, functional impairment, higher risk of relapse, increased self-harming behaviors, and suicidality. An estimated 44% of patients do not respond to two consecutive antidepressant therapies, and 33% do not respond to four. Thirty percent of patients with TRD attempt suicide at least once during their lifetime, which is at least double the lifetime rate in non-resistant depression.
Various treatment tools can be offered and utilized for TRD, including psychotherapy, adjunct pharmacological treatments like lithium, and intensive outpatient treatment or hospitalization in severe cases. Electroconvulsive therapy (ECT) is also known to treat severe depression with acute suicidality. However, this invasive treatment may not be right for many individuals and poses more risks and potential side effects.

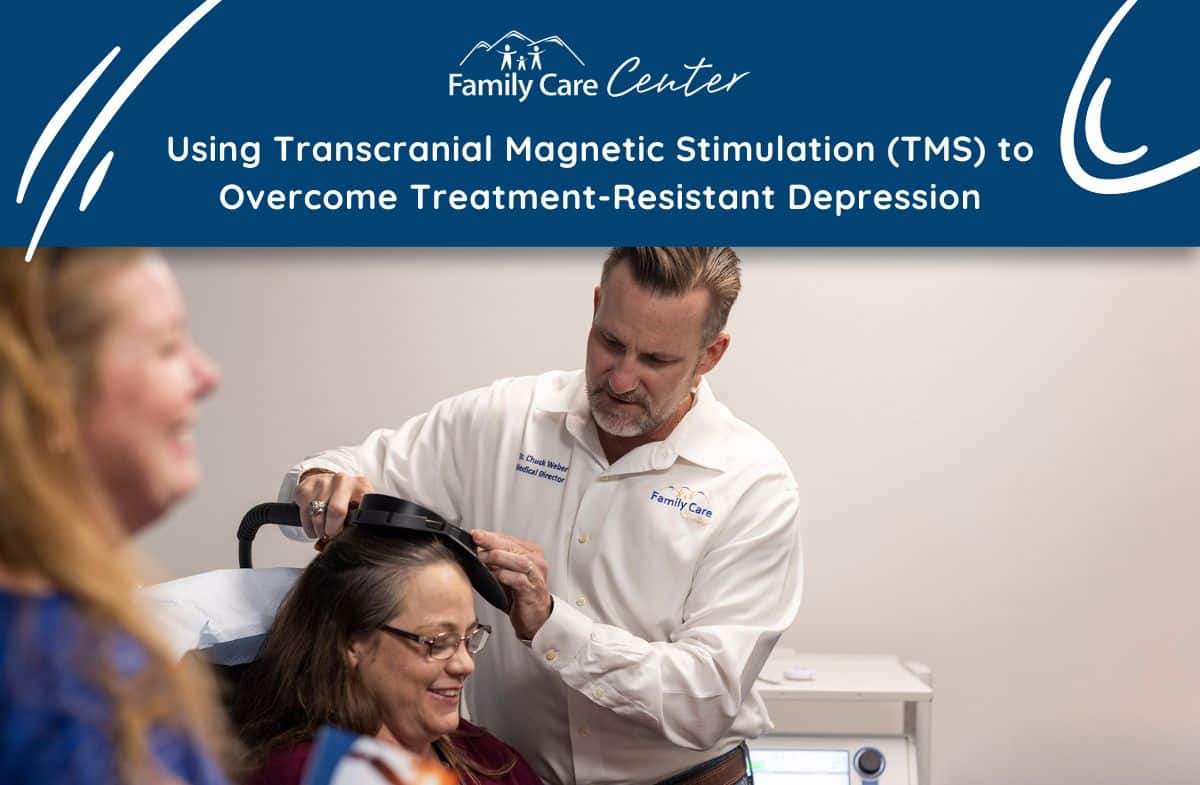
Transcranial Magnetic Stimulation (TMS) Treatment for Depression
There has been increasing research and data supporting Transcranial Magnetic Stimulation (TMS) as an effective and well-tolerated treatment option for TRD. TMS therapy uses painless, repetitive pulsed magnetic fields, similar technology to an MRI. These pulses are usually applied to the Dorsolateral Prefrontal Cortex (DLPFC), a focal region on the superficial cortex of the brain, over several weeks of treatment sessions. This treatment helps alleviate depression and anxiety and improves cognition, energy, and motivation. Clinical studies support several areas of the brain which could alleviate symptoms.
As TMS treatment progresses, energy levels and sleep patterns initially improve. Then feelings of hopelessness and worthlessness associated with depression start dissipating, and for a significant number of patients, they remain in substantial remission thereafter. A recent study has shown that about 1 in 4 people with treatment-resistant depression may achieve full remission with repetitive transcranial magnetic stimulation treatment. Due to our training and experience, FCC providers for TMS have routinely achieved higher response and remission rates.
At Family Care Center, we provide psychotherapy, medication management, and TMS treatment options provided by a top-notch team that collaborates and roots for your treatment and recovery from depression. If you or someone you love has struggled with treatment-resistant depression and would like to know more about TMS, we invite you to schedule a no-cost TMS consultation with our experts to learn about treatment, insurance, and scheduling options.
Reference:
https://alert.psychnews.org/2023/01/study-supports-repetitive-tms-for.html; published on Jan 30, 2023
https://www.nimh.nih.gov/health/statistics/major-depression; updated January 2022